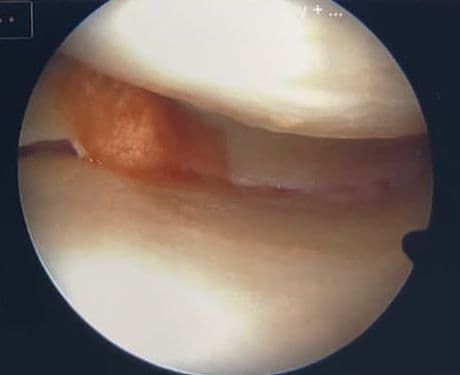
STACi keeps the principle ACi proved: use your own cartilage cells to regrow damaged cartilage. What it changes is how those cells are delivered. Instead of being sealed under a flap of shin tissue, they sit inside a three-dimensional scaffold (a sponge-like structure) that supports cell growth in depth as well as across the surface, much closer to the way natural cartilage is built. There is no need to harvest periosteum from your shin.
That single design change means STACi can do everything ACi does, plus the things ACi cannot. It is suitable for the same patients ACi was designed for, and also for those who would have been turned away from ACi because their defect was too large or too complex. And because the scaffold approach is reliable across joints, STACi is offered for the knee, hip, shoulder, ankle and other joints, not only the knee where ACi has historically been most used.