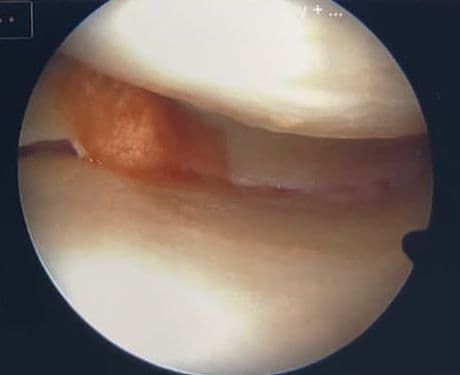
Hallux rigidus and big toe arthritis are very common conditions that limit walking, running and even comfortable shoe wear. The standard surgical answers are cheilectomy, fusion or replacement, each of which trades motion for relief in different ways.
- Osteoplasty reshapes the first MTP joint to restore normal contour.
- Cartilage augmentation is then applied to the prepared surface to restore the joint lining.
- Joint motion is preserved rather than sacrificed, which matters for walking, push-off and balance.
TOAT is a joint-preserving alternative for patients who would otherwise be heading for fusion, where the disease stage and joint anatomy are still amenable.