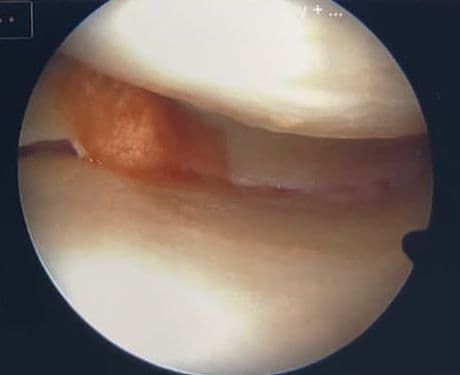
The preserve, repair, regenerate, replace pathway exists because most ankle arthritis patients have more options than they have been told. We work through that pathway with you before replacement is recommended.
- Preserve: activity modification, biomechanical correction, and symptom-relief injections.
- Repair / regenerate: biological injections, AOAT for focal defects, cartilage repair where appropriate.
- Replace: total ankle replacement only when the alternatives have been exhausted or are not realistic.
We do offer ankle replacement, and we do it well, but it sits at the bottom of the list of options because it is irreversible. Come and speak to us before you accept that replacement is the only answer.