




Based on the prestigious and well-renowned Harley Street medical district, London Cartilage Clinic offers several specialised services. We help patients that are looking for reliable alternative solutions to routine healthcare from dedicated professionals without lengthy wait times.
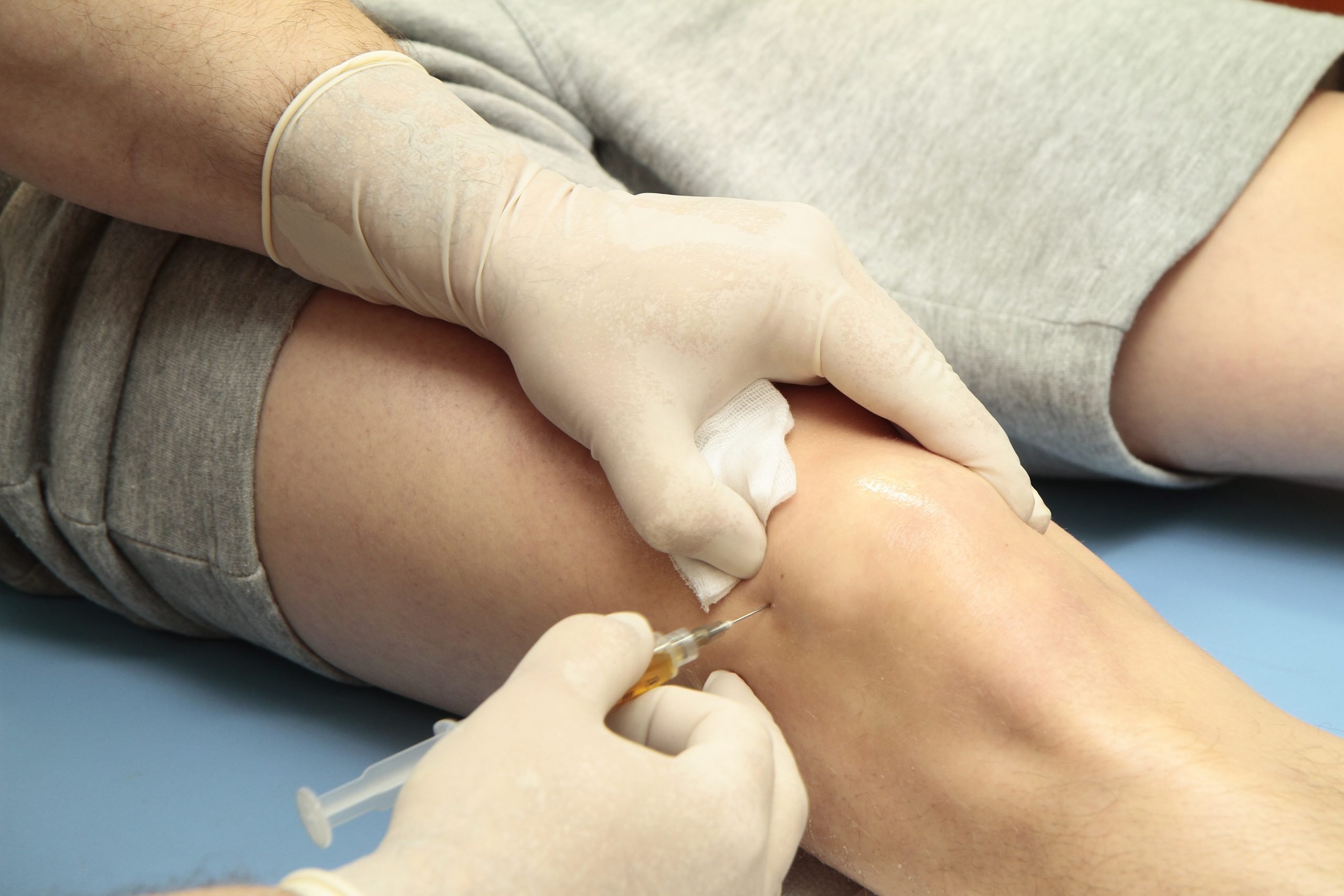
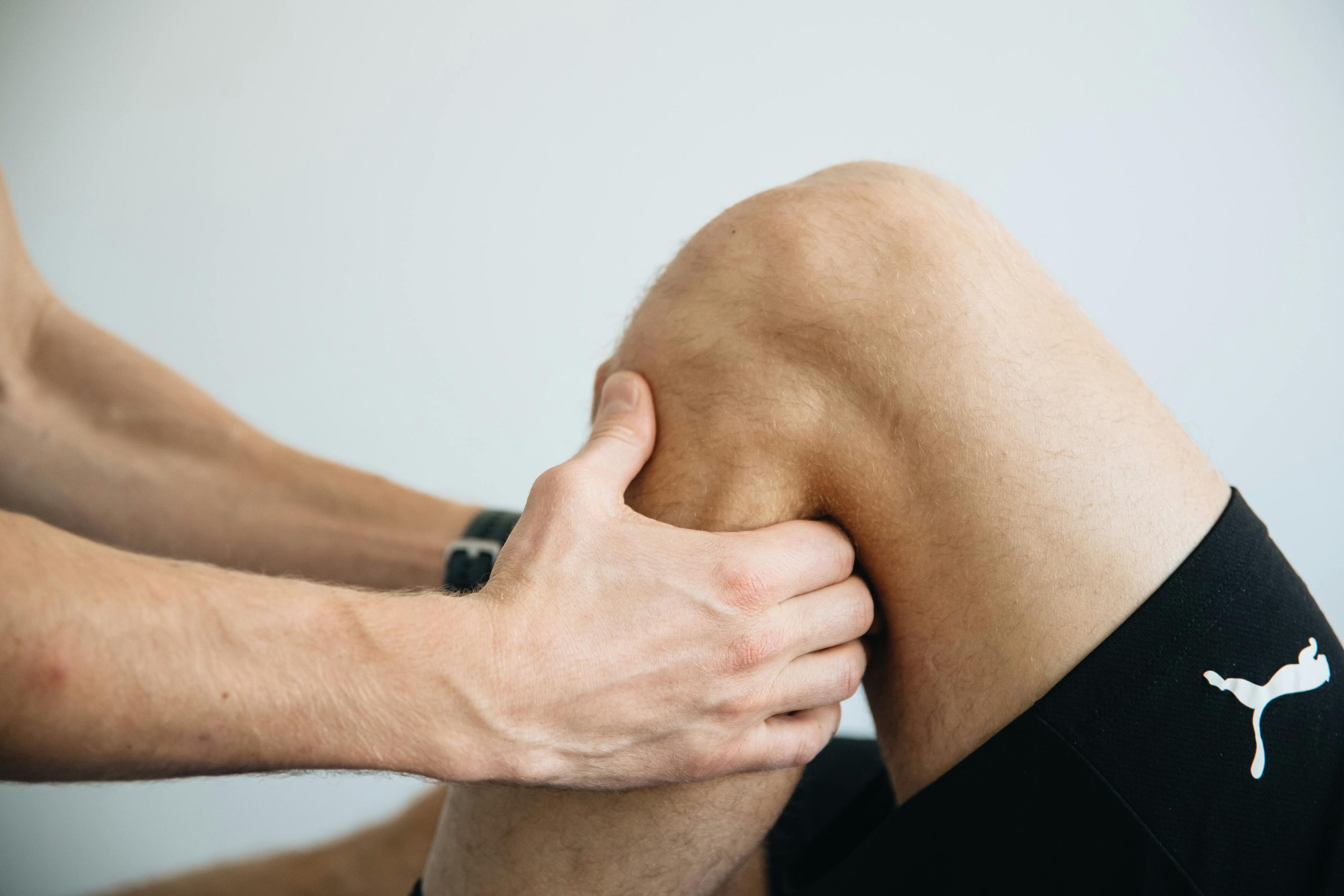
Whether you have a sports injury that is causing pain or are looking to manage symptoms and discomfort caused by a degenerative condition like arthritis, our multidisciplinary team can support you and ensure you receive the highest level of care and treatment.